Govt funding for GP clinics rose to nearly $350 million in 2025
Sign up now: Get ST's newsletters delivered to your inbox

The funds represents an average allocation of more than $140,000 for each clinic, said Health Minister Ong Ye Kung on May 15 at the Singapore Primary Care Conference.
PHOTO: ST FILE
SINGAPORE – General practitioner (GP) clinics received more government funding following the launch of Singapore’s preventive care strategy Healthier SG, as these private clinics have had to play a larger role in delivering preventive and chronic healthcare.
The funds rose from $230 million in 2022 to about $350 million in 2025.
This represents an average allocation of more than $140,000 for each clinic, Health Minister Ong Ye Kung said on May 15 at the Singapore Primary Care Conference.
Singapore is moving towards preventive healthcare interventions, where support is introduced earlier at the community level to delay functional decline and promote healthy longevity.
Under support programmes such as the Community Health Assist Scheme and Healthier SG, the Ministry of Health (MOH) pays grants and service fees directly to GP clinics.
Looking ahead, the trend in increased funding for GP clinics will continue.
“This means that as revenue from medication mark-ups comes down because of competition and other factors, it can be made up, or more than made up, by government payments and service fees for population health,” said Mr Ong, who is also Coordinating Minister for Social Policies.
“But to deliver more preventive and chronic care, clinics will need new capabilities – and new ways of working.”
Many GPs are “solopreneurs”, with one clinician delivering most of the care, he said. But chronic care – especially for patients with more complex needs – takes a team.
Polyclinics have moved towards the “teamlet” care model, where chronic patients are cared for by a team of doctors, nurses and care coordinators.
Under this model of care, a recent internal MOH study found, chronic patients were more likely to keep up with recommended screenings and follow-ups, leading to fewer complications over time, said Mr Ong.

Minister for Health Ong Ye Kung (right) chats with event participants at the Singapore Primary Care Conference on May 15.
ST PHOTO: MARK CHEONG
Primary care costs rose slightly, but savings from fewer hospitalisations and specialist visits more than offset this, he added.
GPs can work towards the teamlet model by being a part of a primary care network, where private clinics collaborate with one another, and also by hiring additional healthcare staff.
GPs’ access to equipment that polyclinics have – such as X-rays, ultrasound or retinal cameras, which need heavy capital investment – will be widened.
MOH will explore ways to enable the clinics’ Healthier SG enrollees to have better access to subsidised ancillary and diagnostic services, either through community health posts (CHPs) or polyclinic services, Mr Ong said.
GPs can also improve chronic care by tapping stronger support in the community.
Over the past few years, MOH has invested in CHPs and active ageing centres (AACs), where seniors can stay active, build social ties and receive lifestyle counselling, as well as frailty assessment and interventions. Agencies such as the Health Promotion Board and People’s Association are also rolling out more healthy lifestyle activities in the community.
GPs can be part of these efforts by connecting residents to the healthy lifestyle activities, as well as coordinating care with AACs or CHPs.
GPs can help to “operate a CHP or partner a CHP to enrol residents in healthcare” and conduct health screening and frailty screening for seniors at an AAC, said Mr Ong.
To facilitate this, MOH has worked with the Housing Board to rethink tenders for new GP clinics in housing estates to give greater weight to care quality, rather than price.
In the past year, eight clinics were tendered out through a price-quality model and have received strong proposals from bidders. Winning price bids have been relatively stable – and at only a fraction of the record high price registered in 2025.
A tender for a GP clinic in Tampines, which closed in early 2025, received the record bid of $52,188, prompting the authorities to come up with the new tender approach for clinics.
Another change in Singapore’s primary care system is the recognition of family medicine as a speciality to support preventive care. Since Nov 1, 2025, more than 220 family medicine specialists have been accredited by the Specialists Accreditation Board, Mr Ong said.
Primary care physicians act as gatekeepers to hospital services, he said.
Historically, primary care in Singapore functioned like “one system, two sectors”, Mr Ong said.
While government-run polyclinics held about 10 per cent of primary care doctors, they shouldered close to half of the chronic workload. Conversely, private GPs, which comprised the bulk of primary care doctors, handled mostly acute cases such as coughs, colds and fevers.
This has changed in recent years. In the community, more preventive care efforts have also sprung up as the population ages.
SingHealth Polyclinics announced at the primary care conference that it has started a trial for an artificial intelligence-powered “brain gym” for seniors with mild cognitive impairment (MCI) to help combat the rising tide of dementia.

A woman participating in interactive, gesture-driven gameplay using fitness apparatus, as part of a “brain gym” session.
PHOTO: SINGHEALTH POLYCLINICS
Users of the automated digital training programme, officially known as the Brain Health Playground, will engage in cognitive and physical activities simultaneously to support brain health and slow cognitive decline.
People with MCI experience noticeable declines in memory or thinking skills but can still perform daily tasks. The condition is commonly recognised as an early stage of dementia.
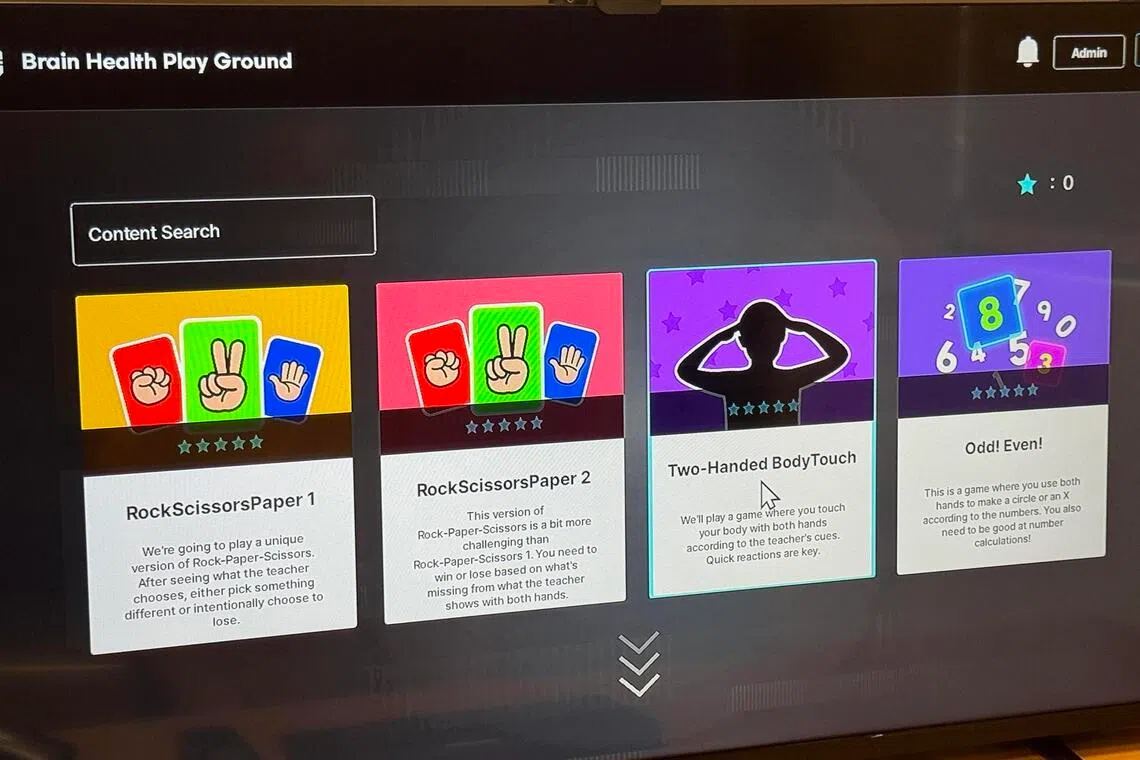
Users of SingHealth Polyclinics’ automated digital training programme will engage in cognitive and physical activities simultaneously to support brain health and slow cognitive decline.
PHOTO: SINGHEALTH POLYCLINICS
The “brain gym” trial, which started in May at Eunos Polyclinic, involves 60 patients aged 60 and above, said Associate Professor Tan Ngiap Chuan, director of research at SingHealth Polyclinics. They have to attend 16 sessions over eight weeks.
SingHealth Polyclinics aims to complete the trial in a year’s time and hopes to deploy it at AACs.
The theme for 2026’s Singapore Primary Care Conference, “Sustainable and Resilient Primary Care”, underscores the need to strengthen primary care capabilities amid evolving healthcare demands.
Organised by SingHealth Polyclinics, together with NHG Polyclinics, National University Polyclinics and the College of Family Physicians Singapore, it drew more than 600 family physicians and GPs.



